Quick Links
Step One: Discover Existing Research »
Step Three: Identify Measures »
As patients, we often evaluate our interactions with the “system” of healthcare innovation and delivery with a simple question: “did it work for me?” This encompasses many issues, including accessibility and availability of the best treatments, how those treatments are delivered, and how they fit with our identity, circumstances and values to achieve the best possible outcomes. Today, there are abundant rankings in health care, and even more measurement, particularly in delivery of care. But we still lack a way to answer the patient’s question: “does it work for me?” FasterCures, a Center of the Milken Institute, has spent the past two years conducting research, convening experts, and beginning to develop an approach to answering that question.
We have all heard that the biomedical innovation ecosystem (i.e., new medical product discovery, development, and access for patients) should be better, faster, and cheaper. In fact, one of the easiest ways to start a conversation is to ask for an example of how the health system fails patients. Here are some examples on just one topic, the relationship of treatments and funding to the disease. For the over 10,000 known diseases, we still only have roughly 500 treatments, and numerous research studies have identified the lack of alignment between the number of patients impacted by a condition and the level of resources aimed at addressing it. In fact, over the past decade from 2008 to 2017, 28 percent of investment from emerging therapeutic companies focused on oncology, while prevalent chronic conditions such as respiratory and cardiovascular garnered only 4 percent and 2 percent respectively. These mismatches are just one example of an area where the system does not align with patient needs.
These problems of low performance or “slow zones” in the system keep the FasterCures team, and many others, up at night. At the same time, we have seen examples where government, industry, researchers, medical professionals and patients have overcome barriers and fast-tracked positive outcomes for patients, creating “hot spots” of innovation and solutions, and we recognize that they represent high performance.
Where does that leave us? When it comes to high and low performance of the innovation ecosystem for patients, we have many examples, but no tools for comparison, knowledge sharing, or monitoring outcomes over time.
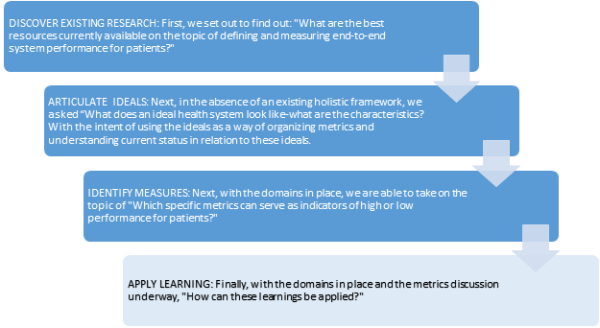
Recognizing this as a challenge squarely aligned with our mission to accelerate medical research and new treatments to patients, FasterCures has engaged with researchers and partner groups with expertise in the biomedical system and patient advocacy. Together, we have embarked on an initiative to find new ways to understand, evaluate, and measure the performance of the biomedical innovation ecosystem for patients, with the development of a “scorecard” as our goal. It is part of our role to identify where the biomedical innovation system is performing well or poorly. For FasterCures, this effort can help us surface opportunities to mobilize and coalesce efforts to address areas where it is not measuring up, and learn from areas where performance is high. For other stakeholders, it provides a novel tool: a framework for looking at performance in a system-wide context. With that in mind, we set out to answer a number of questions in the development of a scorecard, and each answer propelled us to another question. In this series of blog entries, we’ll cover each of the questions addressed in our Biomedical Ecosystem Performance Measurement Initiative.
As we took on these questions, we engaged with expert partners to identify answers. At FasterCures, we know the power of partnership and have worked in lockstep with a diverse set of stakeholders, representing patient groups, government, providers, health system experts, economists, and members of the healthcare industry to address these questions.
Step One: Discover Existing Research
What are the best resources currently available to understand how to measure system performance?
Our first step was to understand what other work has already been done to examine and define performance. As a foundational step, we commissioned Susan Guthrie, PhD at RAND Europe to tackle that question. She and her team of researchers looked far and wide for existing frameworks, indicators, and metrics that we might leverage for our scorecard. The full report is titled, “Existing indicators to measure the biomedical innovation ecosystem: A targeted landscape review for FasterCures.”
What did they find? A gap and an opportunity. The researchers did find interesting models like this one that detail a specific set of dynamic and interactive players. However, they did not find existing frameworks that are commonly used for this purpose: assessing the performance of the biomedical ecosystem end-to-end and evaluating based on how well it works for patients. So, not only is there no comprehensive set of measures, there is not consensus on what aspects of the system should be measured. In addition, existing individual metrics for system performance rarely relate to patient benefit. This paper leads us to the somewhat daunting finding: to accurately determine how it is working for patients, we need more than new measures. We need a new way to look at the biomedical ecosystem holistically through the lens of patient and societal benefit.
In the next blog in this series, we’ll share how we started to look at the next question: what is that new way of looking at the system? How do we define the ideal and identify metrics that reveal where we stand in relationship to the ideals? In the meantime, please share your thoughts in comments: when it comes to our current biomedical ecosystem, what is an example of high or low performance for patients?
Step Two: Articulate Ideals
What does a high-performing health system look like?
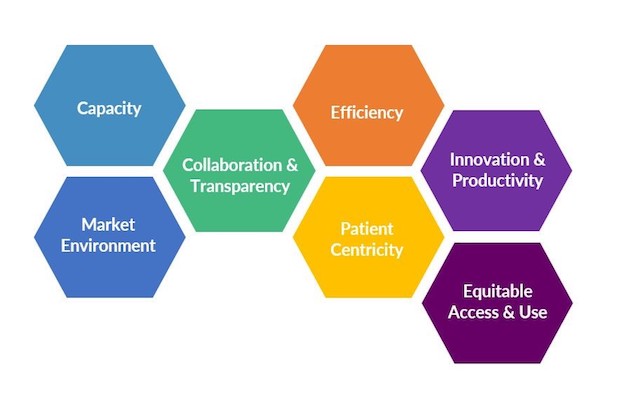
To fill that gap, we decided that our metrics approach would start from defining the vision and purpose of the initiative. The vision agreed upon was a learning biomedical ecosystem that improves health outcomes for all with the purpose to understand and create transparency in the system to optimize its performance for patients. FasterCures then sought to identify attributes of high performance and working to ensure it was holistic. To do so, the group of experts in the working group reviewed a potential set of domains from the study then modified by the FasterCures team. The working group came to consensus that the following domains characterized an ideal, high-performing biomedical innovation ecosystem for patients.
The domains are designed to span the entirety of medical product research and development to payment and patient access, so the categories are broad. They are flexible and allow for interpretation and application. They represent both the ideals of the system, and ably categorize the types of failures to meet the needs of patients. These domains offered an important set of “first principles” on which to build a set of measurements that will allow for a more consistent, holistic view of the performance of the biomedical ecosystem for patients.
Step Three: Identify Measures
With the domains in place, which metrics can serve as indicators of high or low performance for patients?
This framework, designed to articulate the ideal health ecosystem, has presented a useful tool for examining multiple questions about measurement. FasterCures is working with the original working group who helped create the domains, to choose specific metrics to build out the scorecard on a cross-system basis.
At the same time, we have launched an oncology working group to look at measurement specifically through the lens of oncology as a “test case.” The group is co-chaired by Clifford Hudis, MD, FACP, FASCO, CEO of ASCO, and Jeff Allen, Ph.D., President, and CEO of Friends of Cancer Research. The members are drawn from patient advocacy, research, provider, industry, and government representatives, with a focus on cancer specifically. This group has begun to provide input on how the domains are meaningful for cancer specifically and measures that matter most for patients in an oncology scorecard. As part of this program, we are hearing from a range of stakeholders on “hotspots and slow zones,” specific, real-life examples of high and low performance, which help make clear why the scorecard is needed.